
Carole

Carole has had a curve in her spine for most of her adult life. Her GP explained that her spine has a ‘C’ type curve called ‘kyphosis’.
Over the years, her kyphosis has become more pronounced and Carole experiences back and hip pain. She finds that her symptoms interfere with her day-to-day life and prevent her from being hands-on with her grandkids. Carole undertakes her own research and contacts Gold Coast Spine to enquire about how to get an appointment with Dr Scott-Young. Carol is advised that she will need to see her GP first, as a GP referral is required.

Carole visits her GP and they agree it’s time to get some specialist advice. The GP provides her with a specialist referral.

Carole visits Gold Coast Spine to enquire about an appointment and brings her referral with her.
Carole is asked to complete some forms about herself and her condition. She sends the forms to us along with her previous radiology reports.

Gold Coast Spine’s nurse calls Carole for her Nurse Health Check. The nurse collects a full picture of Carole’s history relevant to her spine and general health.

On the day of her appointment with Dr Scott-Young, the nurse checks in again with Carole to update any information since the Nurse Health Check.

Carole then attends her first appointment with Dr Scott-Young. He listens to the history of her condition, examines Carole and reviews her radiology. Dr Scott-Young discusses his views with Carole, answers her questions and lets Carole know what her treatment options are. He explains the reasons why Carole’s spine is collapsing and that she will find that the deformity in her spine will increase with time.

Dr Scott-Young tells Carole that many people are able to manage any discomfort and symptoms with simple measures without surgery. He says that kyphosis correction surgery is complex surgery and, if Carole chose surgery, she would need to carefully consider not only the potential benefits of the surgery but also the significant risks associated with such a large procedure.
He discusses the surgery with Carole and gives her information about the procedure. He also arranges for a Surgical Estimate to be sent to Carole outlining the costs associated with the surgery.
A detailed letter outlining the surgeon’s recommendations goes to Carole’s GP. Each time Dr Scott-Young reviews Carole, he updates her GP in writing.

Carole returns for another appointment with Dr Scott-Young and brings a list of questions about her procedure. She also brings her daughter with her. Carole tells Dr Scott-Young that she would like to proceed with the surgery he has recommended.
Dr Scott-Young reviews her medical history and says that they will need to ensure Carole is fit for surgery before proceeding. Carole is asked to see the physiotherapists at Physio Next Door to get as fit as possible for surgery. Carole is also asked to get clearance from her cardiologist and to be reviewed by a specialist physician.

Carole attends a physiotherapy appointment at Physio Next Door, who assess her and provide Carole with some exercises she can do at home.

Carole sees her cardiologist to ensure her pre-existing cardiac condition is stable and to get the OK for surgery. The cardiologist writes to Dr Scott-Young saying Carole is fit for surgery.

Carole is also referred to a specialist physician, who reviews her other medical conditions and medications. The physician writes to Dr Scott-Young and advises Carole’s medical conditions are well controlled and she is able to proceed with the planned surgery.

Once Dr Scott-Young has received the OK from the other specialists, we contact Carole to arrange another review with Dr Scott-Young.
Carole and her daughter attend the consent appointment with Dr Scott-Young. She asks some more questions she has about the surgery and her recovery. Dr Scott-Young goes over the surgery again, answers her questions and also completes a detailed consent form with Carole.

Carole is then assisted by our Surgical Coordinators to book a surgery date and make the arrangements for her admission to hospital.

Before her surgery, Carole attends the hospital’s pre-admission clinic and has tests performed. The nurse at the clinic answers her questions about what to expect during her hospital stay. Carole also has a pre-operative chest x-ray done.
Carole also attends a pre-admission appointment with Physio Next Door. They will be looking after her in hospital and during her post-operative rehabilitation.
Prior to surgery, Carole clears her bowels with a bowel prep solution.
On the morning of her surgery, Carole arrives at the hospital and is admitted for her surgery.
Her surgeon performs the kyphosis correction procedure with his surgical team.

Following the procedure, Carole spends a night in the intensive care unit so that she is closely monitored.

Carole sticks to soft foods and clear liquids during her immediate post-operative recovery.

Carole is careful to sleep on her side to help her surgical wounds heal.

Carole sees Dr Scott-Young on the ward after her surgery and the specialist physician also visits her post-operatively.

Carole recovers on the ward and begins her post-operative exercises under the supervision of Physio Next Door.

During her recovery, Carole spends some time in the rehabilitation unit of the hospital to ensure that she is ready to go home. The discharge planners at the hospital ensure that Carole will have her daughter to help her during the first few weeks at home. They also confirm she has all the equipment she needs at home to make showering and looking after herself safe.

Two weeks after Carole leaves hospital, she attends her first post-operative appointment with Dr Scott-Young. He is pleased with how she is progressing so far and her wound is healing well. Carole reports that she is moving well and performing all the exercises the physiotherapist has given her.

Carole continues her active recovery by following her physiotherapy programme and increases her activity to include daily walks.

Carole attends her three month post-operative appointment. She is progressing well and has reduced her pain medication. She is committed to her physiotherapy exercises and is cleared to return to usual activities and is encouraged to maintain her fitness.

Carole continues with her active recovery by engaging in a Clinical Pilates programme.

Carole attends her six month post-operative appointment where she is moving well and her recent x-rays show a good result.
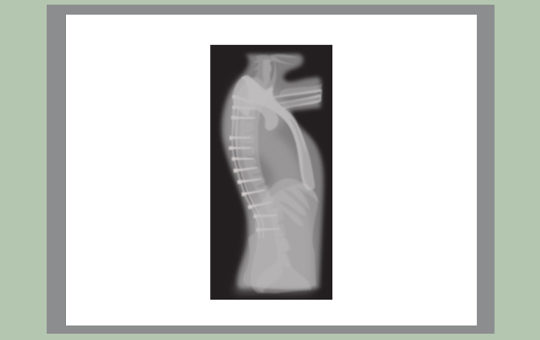
Carole sees her surgeon once again at a 12 month post-operative appointment. Both she and Dr Scott-Young are happy with her result. Her pain is greatly reduced, she has greater mobility and her back, hips and shoulders are significantly straighter.

Carole has an incident 18 months after her surgery when she is bending down to pick up a laundry basket. She feels something ‘pop’ in her back and experiences immediate discomfort in her back. She sees her local GP who contacts Dr Scott-Young, who advises that an x-ray should be performed to see if there is a problem with her spinal fixation.
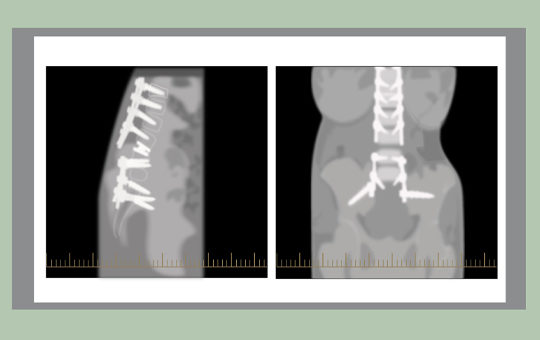
Carole returns to see Dr Scott-Young and he shows her the x-rays of her spinal fixation. He explains that the force that is applied across the implants during bending can sometimes cause the rods to fracture. He notes that this is unusual but does happen.
Arrangements are made for Carole to be admitted to hospital to fix the broken rods. Prior to her admission, Carole is reviewed by her cardiologist and specialist physician to make sure she is fit to proceed with further surgery.

Carole stays in hospital for several days after her surgery and is assisted again by the physiotherapists at Physio Next Door prior to her discharge.

Carole continues another post-operative physiotherapy program after her discharge. Dr Scott-Young reviews her again at 2 weeks post discharge, three months and six months after her revision. At her last visit, Dr Scott-Young reminds Carole not to hesitate to get back in touch should she have any concerns or questions.
